This post may contain affiliate links. As an Amazon Associate, I earn from qualifying purchases.
J-pouch surgery recovery is a full-time job with lots of road bumps along the way
I envisioned being productive during my j-pouch surgery recovery. But like almost all things I envision in my head, life happens and the reality is totally different. What I expected and planned conflicts with my physical and mental realities. I’m exhausted.
Some days, I experience energetic highs that almost have me convinced that I’m completely finished healing. Only to tumble down the hill, wincing and taking notice of all the new swells, bumps, sensitive, and painful areas on my abdomen.
The general trend is upward though. And when I pause to think that recently I was undergoing major surgery, I’m amazed at modern medicine and the body’s almost magical ability to heal.
J-Pouch Surgery Recovery in the Hospital
I was expecting the first hours and days after the surgery to be the hardest and then the later days to start getting easier. But actually, the first days after the surgery was easy. I was pretty heavily medicated and they didn’t make me do a lot.
Waking Up
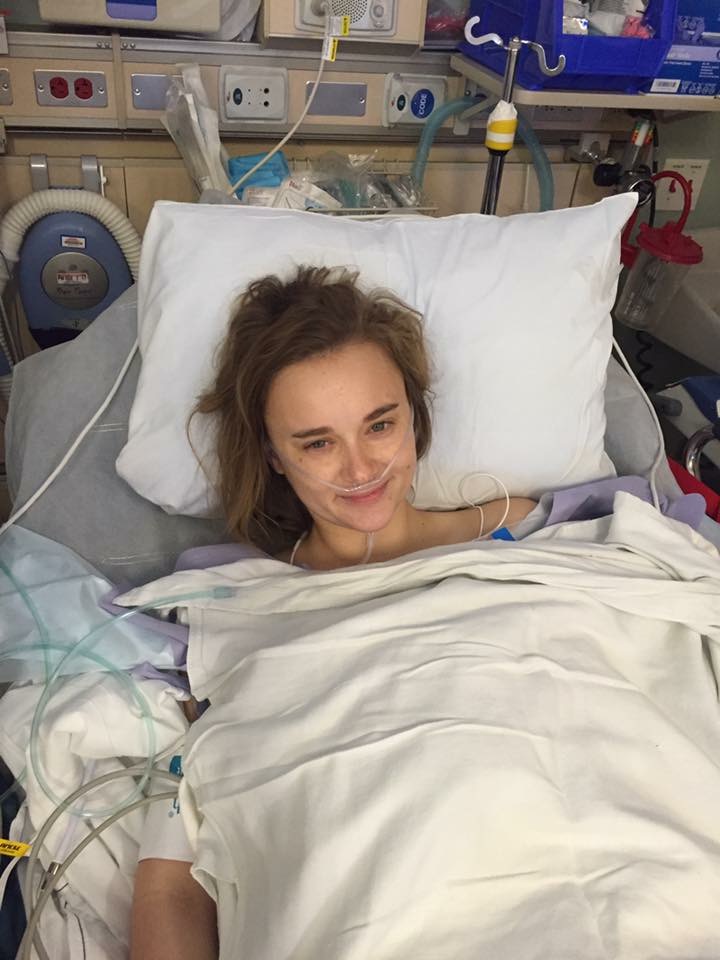
I woke up in the recovery room and to everyone else, appeared to be cognizant. I don’t recall much though. However, I do remember when they transferred me to my room and had to get me on my bed.
In later surgeries, I had an inflatable gurney under me that is blown up, used to help transport me, deflated, and then pulled out from under me.
But not this time. Getting me from one bed to another was an arduous task that forced me to use my non-existent stomach muscles. It was incredibly painful and caused me to groan and cry out in pain.
After getting settled, I drifted in and out of consciousness. It’s hard to get uninterrupted alone time in the hospital, especially after abdominal surgery. Every 10 to 15 minutes someone would come in and check on me, poke me, draw blood, check my blood pressure, or empty my ostomy or urine bag.
The pain medication, liquid Tylenol with occasional doses of an opiate, kept me mostly pain-free. Except for my collar bones. They felt like they had snapped and the bones were sticking out at odd angles.
This painful feeling is caused by the carbon dioxide they pump into your abdomen to inflate it, letting the surgeon see your organs more clearly and give them room to work.
Sharing the Room
I had my surgery done in Walnut Creek, which is an older Kaiser Permanente facility. This meant that the majority of rooms weren’t singles but doubles and it’s the only time I ever had a roommate.
My roommate was brought in late, at least I think so. I still could only turn my head and time blurs together in the hospital.
When they brought her in and got her in the bed, they closed the curtains between us. And when they were situating her, their butts would brush up against the curtain making it billow like there was a wind. I had a trippy dream because of this, thinking I was all alone in a circus tent in the middle of a vast desert.
At one point her pain got really bad and she kept pressing the call button for a nurse but nobody came. I think at that point I said something along the lines of “I’m so sorry they’re not responding” and told her that when that happens to me, I concentrate on breathing in through one nostril and out through the other.
I’m not sure how she responded. Hopefully, she didn’t think it was condescending or a way for me to subtly tell her to shut up.
Walking
Starting on the second and third day my nurses really started making me get up, walk, sit in a chair, eat, and take my medicine on repeat. It was hard work.
One time, after I finally graduated from using my iv pole as a walker, I felt a sneeze coming along. I met a doctor’s eyes in passing and I saw him start to turn back towards me. And then I sneezed and almost collapsed from the pain.
Luckily the wall was right next to me, which I supported myself with. The doctor and a couple nurses came rushing over to check on me and one rolled their chair over.
Post J-Pouch Surgery Challenges
After being discharged from the hospital, the healing process continued, mostly in a 1-step-forward, 2-steps-back format. The challenges I faced included:
- Bladder problems
- Dehydration
- Exhaustion
- Healing stitches and scars
- Pain and emotions
- Adjusting to life with a stoma and ostomy bag
Nonfunctioning Bladder
For a full two weeks after my colon was removed, my bladder wasn’t working. Sometimes after surgery, due to the lingering effects of anesthesia and shock from the trauma of surgery, organs take a while to re-start. In my case, it was my bladder.
Nurses took the catheter out once while I was in the hospital but I soon discovered, with a near bursting bladder, that it wasn’t working. A nurse had to put another catheter in and a doctor picked a timeframe for me to get it removed.
Catheter Woes
The catheter made everything harder: sleeping at night, taking a shower, walking, and sitting. There was no comfortable position to get in. I felt it was slowing down my recovery, especially with my walking habits.
Walking is extremely beneficial for recovering from hospital stays. But every time I went on a walk, the catheter would start to hurt and burn.
At night, my mom had to hook me up to a larger overnight catheter bag and arrange it to make sure it was low enough for the urine to flow down. If a catheter bag is too high, the flow of urine will flow back up the tube, which can cause infections.
Whenever I took a shower, I had to keep the leg the bag was attached to out of the tub while simultaneously making sure the bag and tubbing stayed low.
Catheter Removal
To check if my bladder was ready at the end of the two weeks, I got an ultrasound done. You go into the appointment with a full bladder and they take an image before removing the catheter. Then the nurse removes the catheter and you try to go to the bathroom. If you have success, they then take a second image to make sure you completely emptied your bladder.
Obviously if you aren’t able to go to the bathroom, the catheter gets put back in. But it also gets put back in if you can’t empty your bladder completely, since that can cause infections.
Luckily, I passed the test and got the catheter taken out. I immediately started to feel better.
Dehydration
I had a hard time with dehydration during my j-pouch surgery recovery. There were a lot of days where I experienced a dizzy and tingly feeling whenever I got up.
My ostomy nurse told me that I needed to supplement my water consumption with electrolyte drinks.
Your colon is responsible for absorbing the rest of the water and other nutrients left behind by the small intestine. This both helps stool solidify and extracts more nutrients for the body.
I’ve always enjoyed plain water, so trying to get used to drinking sports drinks was tough. My dehydration also didn’t help with my exhaustion problems.
Exhaustion
J-pouch surgery recovery, dehydration, and coming completely off prednisone were all factors in my exhaustion problem. My exhaustion was no joke. It was a new level for me. I had no freedom and needed help doing everything.
My mom acted as my nurse the second I got home. She would move, fetch, and assist me in almost everything. Because I kept getting overwhelmed with daily life.
Opening sliding glass doors or drawers that were too low or too heavy, getting into cars, taking showers, working at the computer, sitting, walking, standing—all of it was exhausting.
The first 4 days my voice was practically gone. Some of this was because the anesthesiologist intubated me. But also, I didn’t have the strength and energy to get sound out.
Often, I would have a couple of days with normal energy levels and then reach a plateau in my healing process. And that’s when another wave of exhaustion and fatigue would hit me.
No More Prednisone Energy
Since deciding to have surgery, I was slowing being weaned off prednisone. By June 10, 2016, I was on only 10 mg and by June 29, I was off it completely.
Prednisone gives me a lot of manic energy and whenever I start coming off it, my energy drops drastically. This also added to my exhaustion levels.
Coming off of it caused me to have skin problems too. My whole body was extremely itchy and I was covered in hives. The extreme summer heat sapped all my energy, made my skin issues worse, and generally made me a grump.
Stitches and Scars
My stomach doesn’t feel like my stomach.
The stitches, scars, swollen lumps, and holes in my stomach alienate me from my own body. It’s a new landscape, a new world, and it’s all a little weird.
On my left side, I have a small hole where my drain was. A drain is a small tube that’s kept inside you after surgery to drain fluid. Your surgeon removes it after a certain time period, generally when output has greatly reduced.
When my surgeon removed mine, it felt very strange. It reminded me of when you pull a big weed out of the dirt and the roots have a good grip on the soil.
On my right side, I have an opening in my abdominal wall, where my stoma, a part of my small intestine, is sticking out. It’s covered by my ostomy bag, which also covers my belly button.
I can’t tell you how strange it is to not see your belly button every day. A belly button is so human-an indicator that you were born.

There are a couple of small laparoscopic pinpoint scars scattered across my belly and one large incision from my lower navel all the way down to my groin.
I feel uncomfortable in my own skin and clothes are extremely annoying. Most hit, rub, and put pressure on my stitches and forming scar tissue.
Pain and Emotions
So much pain. And so many emotions. In the j-pouch surgery recovery process, I’ve had a couple of bad moments that I’m not too proud.
I’ve broken down and cried. There has been some screaming and bursts of irritability and anger. Sometimes I feel downright mean, like I’m turning into a different person. There have been days where I feel really scared.
Some of these emotions are directly connected to my pain and others are their own wound.
Everything about my abdomen, my stoma, and my j-pouch is just so hard. It feels different. It looks different. And I’m trying not to freak out.
Every time I try something new, I get a little worried and question what’s going to happen. I stare at my bag and stoma looking for what’s coming out and whether it is going to be okay.
Being overwhelmed with my pain
In some ways I’m overwhelmed with my pain. Not the pain level necessary, but the unfamiliarity of it.
You can feel better about your pain when you can pinpoint what’s wrong and why. But there are so many issues below my waist that it can be hard to determine what’s going wrong.
There’s swelling, extreme soreness on certain parts of my stomach, very hard spots, very soft spots and I don’t know what any of it means.
The pain impacts every portion of my life. Little actions that you do unconsciously have the potential to cause great pain.
When I wake up in the morning, I tend to do a full body stretch. I do it without thinking and couldn’t stop myself. It hurt extremely bad and woke me up in the worst way.
Two weeks after having my colon removed it still hurt to laugh. I’ve taken to avoiding anything I find funny because trying to stop a laugh is almost as painful as laughing.
Going to the bathroom sucks because there is so much tension. I have to breathe deeply in order to relax enough to urinate. Only I have to concentrate very hard to pinpoint where my muscles are and how to relax them. Everything down below my waist feels mushed together and I can’t differentiate which muscles do what.
All my clothes press against my scars and when my belly swells, I feel suffocated by them. I’ve never wanted to walk around nude in my life, but it has a certain appeal right now.
There is no position I can arrange myself in that doesn’t bother some part of my body right now. It all hurts.
Tired of feeling helpless
In the hospital I had to rely completely on the nurses. That can be an incredibly humbling experience.
Having knowledge of your own body and being able to control it and understand it is incredibly powerful. It’s not until you lose that ability that you recognize just how powerful it is.
At one point, when I was still in the hospital, I noticed I was bleeding. But my stomach was so swollen and I was so sore from the surgery that I couldn’t bend enough to see where the blood was coming from.
I had all male nurses that day and when they asked if it was period blood, I had to tell them that I didn’t know.
Not being able to answer a basic question about my body embarrassed me. I felt like a little girl again listening to older girls talking about bleeding and having no clue what they were talking about.
I had to wait all day for the (male) physician’s assistant to come and examine me to determine if the blood was coming from my anus (surgical bleeding), vagina, or urethra (bleeding from the catheter).
The whole situation was a little funny. I just wanted someone to look at my vagina and tell me that I was on my period. But it also made me feel incredibly helpless.
Having to rely on other people for everything
And that’s how the whole j-pouch surgery recovery has been. I’ve had to rely on other people to do the most basic of tasks for me because I can’t.
From taking showers, making sure I eat, helping me get up or sit down, getting my clothes ready for me, picking up anything over ten pounds, walking with me, or putting on my shoes—I’m so tired of asking for help. It’s great that I have people I can ask but I want to do everything by myself again.
Stoma Life
I have a whole post dedicated to this topic, so you can read about it here. It’s part of my j-pouch surgery recovery and it adds another level of physical challenges like
- Skin problems near the stoma
- Blockages
- Bag leaks
- Travel complications
It also adds mental challenges to my recovery like
- Feeling like I smell or that I’m dirty
- Decrease in self-confidence
- Self-loathing
- Feelings of anger, fear, and shame
Read Stoma Life: My 3 Months with an Ostomy
Facebook Live Videos
Some of what I wrote here I talk about in these Facebook Live videos, which you can watch below.
My Whole UC Story
You can read my ulcerative colitis story in order or you can browse all my ulcerative colitis and health-related posts here:
- My UC Story: where and when my ulcerative colitis symptoms first started
- Part I – The Beginning of My UC Story: what my symptoms were and the struggles I had getting health care
- Part II – UC Diagnosis and Adjustment: how I was diagnosed and how I struggled to adjust to living with ulcerative colitis (including diet experiments, and getting frustrated with doctors not listening to me)
- Part III – UC and Severe Back Pain: my ongoing struggle with severe back pain + getting a new GI doctor that listened to me and who sent me to a rheumatologist
- Part IV – Sacroiliitis Diagnosis and UC Remission: getting diagnosed with sacroiliitis, getting on Remicade, and finally going into remission (with both my UC and joint disease)
- Part V – The Second UC Flare: my slowly deteriorating health, worsening symptoms, colonoscopy, and my first ER visit
- Part VI – First Hospitalization: my first hospitalization from my second ulcerative colitis flare and my experience with bowel rest and edema (swelling from fluid).
- Part VII – Being on Prednisone for My Second UC Flare Recovery: being on Prednisone for the first time and the various effects it had on my mind and body + adding mercaptopurine (6MP) and allopurinol to my daily routine
- Part VIII – Third UC Flare and Second ER Visit: my third UC Flare experience, symptoms, ER visit, and tests and procedures (CT scan, proctoscopy, etc.)
- Part IX – Recovering From Two Consecutive Flares: being released from the ER and the struggles of recovering from two consecutive UC flares (three months apart)
- UC Planning Realities: Trying to Write and Defend a Thesis: the difficulties in making long-term plans with UC and trying to meet thesis deadlines while in a flare
- Post UC Flare Routine: my post UC flare routine that helped me manage my physical and emotional symptoms
- Body Image and Mental Health with UC: Stop telling me I look great: the connection between body image and mental health and how my experience with ulcerative colitis has complicated my relationship with the two
- Making Travel Plans with UC: the difficulties in making travel plans with UC
- The Nightmare of Ulcerative Colitis: I compare a reoccurring childhood nightmare I had to the nightmare of ulcerative colitis
- Part X – Fourth UC Flare: My fourth UC flare experience, symptoms, hospitalization, tests, procedures, next treatment steps, and recovery
- Hanging Out in Limbo: waiting for experts to weigh in on my situation is like hanging out in limbo – I have no new treatment plan and I don’t know what the future holds
- Part XI – How Losing My Colon is a Transformation and Not a Loss: I’m losing my colon soon. But read about how this is a transformation and not a loss and how I made the decision to remove my colon
- You’ve Just Crossed Over into the Prednisone: Being on prednisone is a lot like being in the Twilight Zone. Things aren’t always what they seem, it can be hard to navigate and understand your surroundings, and often times you feel like you might never come back. Or the even scarier thought: that you might not ever want to come back.
- Recovery Reads: a list of some of my favorite books to read while recovering from UC flares, hospitalizations, and surgeries
- Pre-Surgery Jitters: my pre-surgery jitters in the days leading up to my j-pouch surgery on May 20, 2016, and how I distracted and pampered myself
- Part XII – J-Pouch Surgery: what my j-pouch surgery (proctocolectomy with ileal pouch-anal anastomosis) was like, including prep, surgery, and recovery
- J-Pouch Surgery Recovery: j-pouch surgery recovery is a full-time job with lots of road bumps along the way including bladder problems, dehydration, exhaustion, healing stitches and scars, pain and emotions, and adjusting to life with a stoma and ostomy bag
- Stoma Life: what my stoma life, the three months I lived with an ostomy bag, was like, including the physical and mental adjustments I went through, procedures, and what travel was like
- Part XIII – Pancreatitis: my struggle with pancreatitis including symptoms, tests, my ER and hospital stay, pain management, post-discharge recovery, and pre-op prep
- Part XIV – Ileostomy Takedown Surgery: how my ileostomy takedown surgery went, including prep, the surgery, hospital recovery, and complications
- Part XV – Post Operative Ileus Complications: my painful and scary experience with post operative ileus complications left me very weak, under 100 pounds, malnourished, and very close to death’s door
- Surgery Recovery and Diet Problems: Physical and diet difficulties from post-surgery recovery and complications from pancreatitis, post-operative ileus, and pouchitis
- Everything is Shiny and New
- Hitting the Wall and The Privilege of Scars and Wrinkles
- Experiencing Loss and The Power and Comfort of Creativity
- Hauntings, Superstitions, and Giving Back: Reflecting on Being Hospital Free for 2 Years

